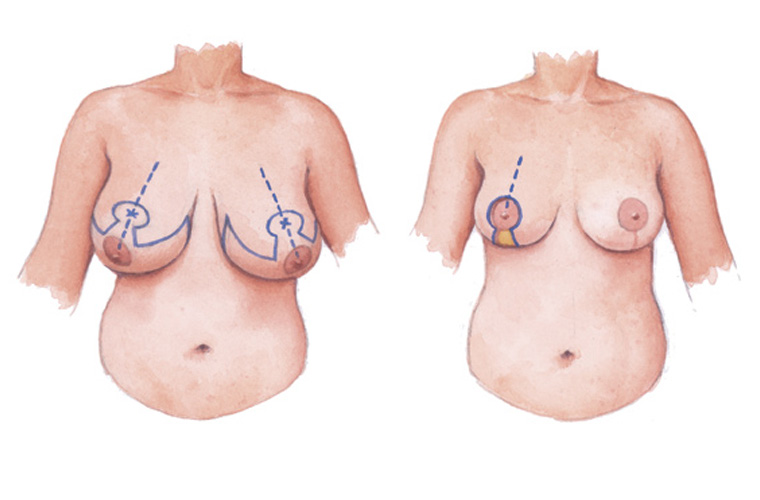
Reduction
Breast reduction is a surgical procedure performed under general anaesthetic to reduce the size and sometimes improve the shape of large breasts.
Why have a breast reduction
Large breasts can cause various physical problems including; back/shoulder/neck ache, poor posture, migraines, chafing and sometimes fungal infection of the skin under the breast. Large breasts can also cause psychological distress, as it can be difficult to find suitable bras and clothing to fit. It can also make everyday activities difficult and stop you participating in some sports. If the size of your breasts is causing you problems, a breast reduction might be considered.
What does it involve?
If you are considering a breast reduction you should make an appointment with your GP whom can refer you to a Plastic Surgeon. If you fall within the criteria to have breast reduction within the NHS, you will be under the care of a Consultant Plastic Surgeon and their team. The funding criteria mean that only women who are below a certain weight and who are expected to have a minimum amount of tissue removed will receive funding from the NHS. If you are a smoker, you will be asked to stop smoking prior to your surgery, as smoking can cause problems with wound healing and can delay your recovery and affect the outcome of your surgery. You will have photographs before and after the operation which will be kept confidentially.
At your first visit to the outpatient department you will be seen by the medical team and your problems discussed and then the benefits and risks of surgery outlined, if suitable. Classic symptoms that may be helped by breast reduction surgery include:
- Neck ache
- Upper back ache
- Poor Posture
- Shoulder grooving or bruising
- Skin rashes below the breast
- Breast Asymmetry
- Droopy Breasts
- Difficulty exercising
- Difficulty finding appropriate clothing or bras
- Difficulty with physical occupations
- Embarrassment, emotional and psychological issues
At St Andrew’s Centre we also provide a consultation with the breast reconstruction nurses who will discuss the case further and show you some pictures.
The Procedure
On the day of admission to hospital you will be seen by the operating surgeon and again the procedure will be explained to you detailing the benefits and risks. Once you are happy to proceed you will be asked to sign a consent form agreeing to go ahead with the surgery. The surgeon will use a marker pen to draw on you the new position of your breasts prior to going to theatre.
Some breast tissue, excess fat and skin will be removed and your surgeon will reshape your breast and lift your nipple so it is in a higher position. The operation usually lasts 2-3 hours (approx) and you will spend some time in the recovery area before going back to the ward. Usually you will have a drain in each breast which will drain away any excess fluid from the operation site. The drain will be removed on the surgeon’s instruction, usually 2-3 days post op. You can expect to have a 2-3 night (approx) stay in hospital. You will usually have dissolvable stitches under the skin with glue over the top of your surgical wounds. The glue should flake away after a couple of weeks. You may have dressings on your breasts post operatively. Most surgeons prefer you to wear a non-wired sports bra immediately post op, which will be applied in theatre.
You will be monitored on the ward by the nursing staff who will check your breasts and nipples regularly, and monitor your drains. You will usually be awake when you get back to the ward and can commence drinking sips of water if the surgical team are satisfied. You will usually be allowed to eat and drink a few hours post op, depending on your progress. If there are any concerns, you may remain nil by mouth until the surgeon has reviewed you. It may be necessary to take you back to theatre should there be any concerns with your breasts post operatively but this is uncommon. You will usually have an oxygen mask over your nose and mouth, which the nursing staff can remove once you are fully awake and alert and your oxygen levels are satisfactory.
You should remain on your bed for at least four hours post op, and only get out of bed for the first time with the assistance of the nursing staff. You will be offered regular pain relief (analgesia) and you may be prescribed antibiotics as a precaution, which will usually be given intravenously (IV) then tablet form if you require them. You must inform the nurses if you take any regular medication which should be prescribed on your prescription chart. You should be able to shower the day after surgery, unless you have dressings which need to stay dry; you will be advised of this on the ward.
Benefits of breast reduction
Some women report a rapid improvement in their posture and relief of back ache. You should find it easier to find bras and clothing to fit. There should be no further problems with the skin under the breast.
What to expect in the weeks after surgery
You may find yourself feeling quite tired up to two weeks post op, which is all part of your recovery. You may require analgesia 1-2 weeks post op, particularly an anti-inflammatory, to help reduce the swelling. The swelling and bruising of your breasts can take up to 6 weeks to subside, by which time your operation wounds should be fully healed. You will be required to wear a non-wired sports bra day and night for 6 weeks post op.After surgery your breasts may appear very high and firm but they will gradually take on a more natural shape and become softer over the next 3-4 months. You may experience altered or loss of sensation of the nipples, which may or may not return. Very occasionally due to other contributing factors i.e. smoking or medical problems, for instance diabetes, the nipple may not survive. In some circumstances due to the nature of the surgery around the nipples you may not be able to breastfeed in the future. You should receive an appointment to attend the Nurse Led Breast Clinic or dressing clinic for a wound check approx one week after discharge. You may notice your wounds appear pinkish red initially, this maybe due to wound healing and is normal, if your wounds appear red and the redness spreads onto the surrounding skin or you see a yellow/green discharge please phone the ward. You should also receive an appointment to see your Consultant and their team; this may be up to 3-4 months post op. You will be left with scars once the wounds are fully healed and you can massage the scars with a mild moisturiser (E45/Aqueous Cream) 2-3 times daily to help reduce their appearance.
Going back to work and activities
Depending on your job and the progress of your wound healing, you should be able to go back to work 2 weeks post op. It is advised to avoid driving for 2 weeks and only start driving again if you are comfortable wearing a seatbelt and can react quickly in an emergency situation. We advise no excessive arm movements, no ironing, no vacuuming or heavy lifting (over 10lbs approx) etc for the first 2 weeks. Avoid sports activities e.g. weights, gym, aerobics, swimming for 6 weeks to prevent pulling your chest muscles. Also avoid bathing until your wounds are fully healed.
And finally...
A breast reduction procedure will make your breasts smaller and is only suitable for certain women. You should consider the options carefully and have realistic expectations about the results.
Due to strict NHS guidelines and service restrictions, it is not always possible to perform this type of surgery under the NHS. There are strict provision criteria, such as body mass index and clinical priority, which need to be met and these should be discussed with your GP or surgeon before a decision can be made to perform such procedures.
Other Procedures
Please go through the information below in your own time to help your understanding of the options available.